Editor’s note: Joachim Osur is the Vice Chancellor of Amref International University. The article reflects the author’s opinions and not necessarily the views of CGTN.
As the world moves towards a post-COVID future, African countries are faced with a formidable challenge: how to make health care systems resilient in the face of crippling shortcomings in the continent’s healthcare workforce that have left the most vulnerable exposed to the injustices of an inequitable health system.
While some countries have called for increased investment in Africa’s healthcare workforce, efforts to narrow the gap between our health needs and the workforce available to meet these needs are yet to be scaled up to impact health outcomes. To meet the fast-approaching Sustainable Development Goals (SDGs), Africa must renew its focus on building resilient health care systems powered by a workforce that is responsive to today’s needs and equipped to navigate tomorrow’s challenges.
Such a workforce is attuned to the requirements of those receiving care, and those delivering it. It is agile and considers the context in which health services are sought and delivered, taking into account sociocultural nuances while at the same time leveraging new medical knowledge and technologies to revolutionize health care delivery. A fit-for-purpose health workforce believes that health care, at its core, is a people business.
To understand the shifts that need to occur within Africa’s health systems to meet evolving needs, we must consider three interlinked realities.
Firstly, for Africa’s health systems to address the needs of the changing world, they must be tailored to achieve their purpose and be supported by well-trained, well-remunerated, highly motivated and equitably distributed health care workers.
According to the 2016 World Health Organization (WHO) Global Strategy on Human Resources for Health, Africa had an average of 1.3 health care workers per 1,000 people in 2015, significantly less than the 4.5 per 1,000 needed to meet the SDGs. This situation is compounded by insufficient skills, brain drain and gaps in service coverage, all of which must be addressed to achieve health care for all.
Secondly, Africa’s primary health care needs continue to evolve. Over the past few decades, the continent has lost millions of lives to HIV/AIDs, malaria, tuberculosis and vaccine-preventable diseases such as measles and yellow fever. However, WHO projects that by 2030, chronic diseases such as cancer, heart disease and kidney failure will account for approximately 42 percent of all deaths in Africa. It is therefore prudent to ensure that systems are in place to address the situation appropriately through stronger primary health care mechanisms and specialized training in fields such as oncology, cardiology and nephrology, among others.
Thirdly, there is an urgent need to update training curricula for health care workers, featuring relevant content on both traditional and contemporary approaches to care. Investment in a highly skilled health care workforce inclusive of community health care workers and traditional healers capable of gleaning knowledge from traditional African medicine and fusing it with modern medicine would be a boost to the attainment of health goals.
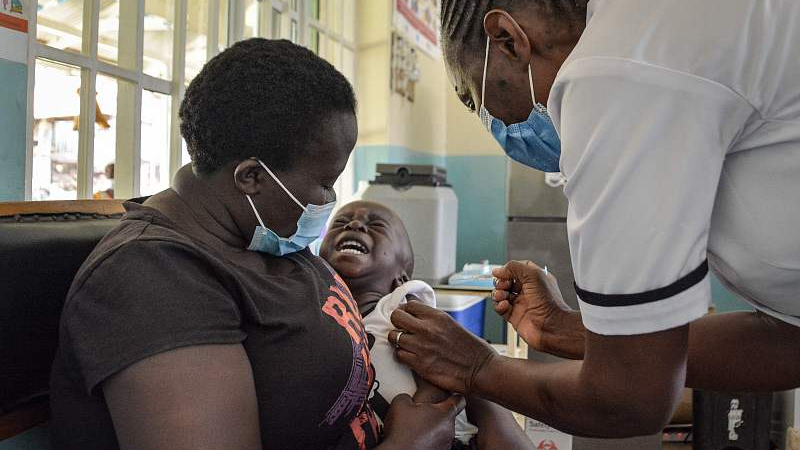
A child gets a malaria vaccination at Yala Sub-County hospital, Yala, Kenya, October 7, 2021. /CFP
By integrating African traditional medicine into our health systems, we can provide more affordable and accessible health care solutions and connect more people to the health care system. In recognition of this, institutions such as Amref International University (AMIU) are now offering courses that feature modules in traditional and complementary medicine, which has been recognised by WHO for its important role in treating chronic illnesses and improving the quality of life for those suffering from minor illness or certain incurable diseases.
Additionally, African countries must make concerted efforts to stay up to date with the latest advances in medical knowledge and technology. Despite often working in resource-poor settings African scientists have proven time and again that they can make greater contributions to health and science given the right tools. Closing knowledge gaps through capacity building and investment in research and development to attract, develop and nurture critical skills along the health value chain is key to bolstering equitable health care delivery and homegrown innovation.
Beyond this, Africa must create absorptive capacity to ensure our abundance of trained health care professionals is retained on the continent. We need to formulate regulatory frameworks to govern and promote health care workforce labor movement within the region, and to strengthen the policy environment for increased investment in shared learning through exchange programs, research, innovation, and entrepreneurship within the health sector. This is especially critical to stem the medical brain drain that is depriving countries of much-needed human resources at a time when competition for trained medical personnel is pitting wealthy countries against their low- and middle-income counterparts, to the detriment of vulnerable populations in many African countries.
The COVID-19 pandemic has taught us that we cannot afford to put our health in the hands of others. Africa must begin to take responsibility for its own health agenda. Strengthening our health care systems by investing in a fit-for-purpose health workforce is a key first step towards achieving our shared health goals.
Article first published news.cgtn.com
